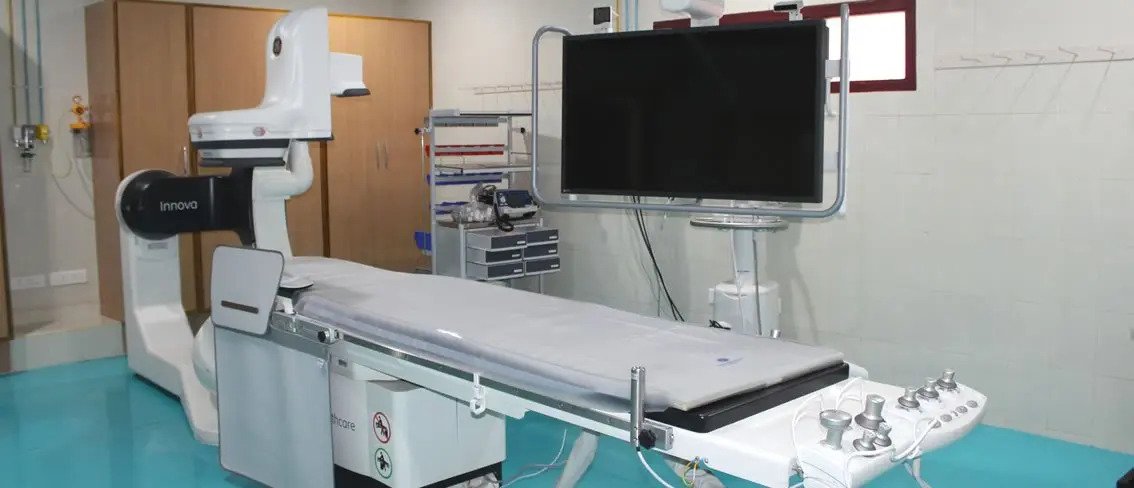
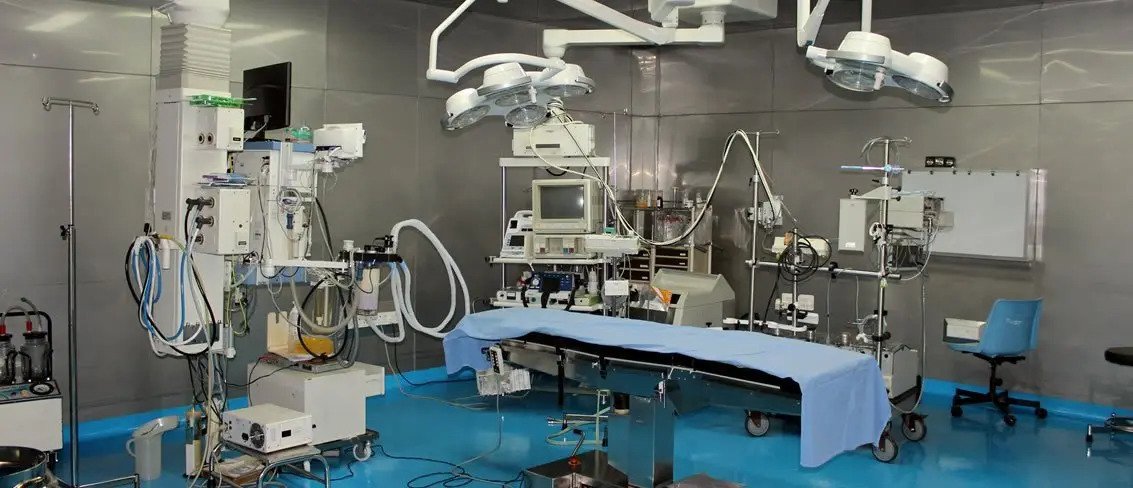
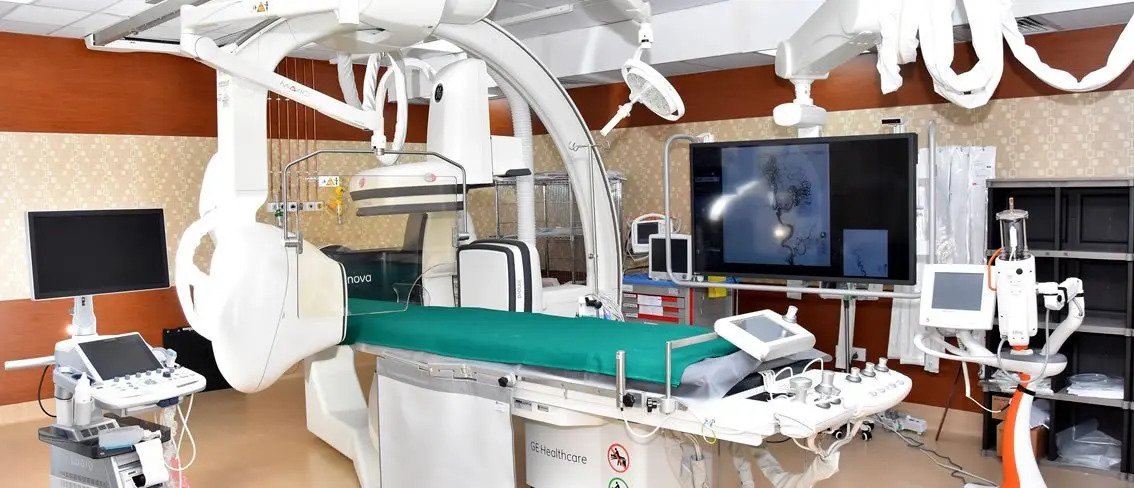
When a coronary artery is blocked (partially or completely), it can cause Ischemic Heart Disease (IHD), Coronary Artery Disease (CAD) as manifested by chest pain (angina). In such a situation it is necessary to carry out coronary artery bypass surgery. Most people have heard of ‘a bypass’ but aren’t too sure what it is.
In short, surgeons use a vein or artery from another part of the body to create a ‘bypass’ so that the blood may flow to the blocked coronary artery. Before performing the
bypass surgery for heart, the patient is put under general anesthesia and the surgeons begin by making an incision in the middle of the chest. The breastbone is separated in order to create an opening through which the heart region may be accessed.
At this point, most patients are put on a bypass pump or heart-lung bypass machine. This is known as an on-pump coronary artery bypass. Essentially, all the work of the heart and lungs is then done by the machine, for the duration of the procedure. It adds oxygen to the blood before circulation to the body and then removes carbon dioxide from the blood as it returns.
The cardiothoracic surgeon then takes a vein or artery from another part of the body. This is fashioned into a bypass wherein one end is connected to the coronary artery while the other connects to the aorta. This allows blood to flow around the blocked section so normal circulation is restored. Some of the common veins and arteries used as a graft in the procedure are the saphenous vein (from the leg), the radial artery (from the wrist), and the internal mammary artery or IMA (which lies in the chest and is already connected to a branch of the aorta).
When the procedure is complete, the breastbone is closed with steel wires (which will remain in the body) and the chest with stitches.
In some cases a patient may not be put on a bypass machine. In these instances, the coronary bypass surgery treatment is done while the heart is still beating. This procedure is known as an off-pump coronary artery bypass (OPCAB). This is a far more complex and technically challenging procedure. But, the benefits to the patient can be quicker recovery, fewer blood transfusions, a shorter stay in the hospital, and even fewer complications in terms of the response of the immune system.
At Sri Ramakrishna Hospital, best cardiothoracic surgeons in Coimbatore are well equipped with the technical expertise to perform both procedures and a vast number of patients have benefitted from our expertise.
Minimally Invasive Coronary Artery Bypass Surgery(MIDCAB)
Just like off-pump coronary artery bypass surgery, minimally invasive direct coronary artery bypass (MIDCAB) surgery is performed on a beating heart i.e. no heart-lung bypass machine is used. The typical coronary bypass requires a large, ten to twelve inch incision on the chest in order to separate the breastbone. MIDCAB on the other hand employs either one incision of three to five inches between the the ribs or many small incisions. During the process, the heart is still beating so it is slowed using medication and stabilised using a special system.
An incision is made on the left side of the chest, between the ribs. Then muscle tissue is spread apart and a piece of the costal cartilage (front part of the rib) is removed. This allows the surgeon to access and ‘prepare’ an artery on the chest wall. One which is situated next to the blocked artery. Then the surgeon connects the prepared artery to the blocked artery.
This process can only be used on a maximum of two coronary arteries and even then, only if they are situated in a way as to make it possible. For more blocked arteries the conventional methods are recommended.
Minimally invasive direct coronary artery bypass has many advantages. Given the smaller incisions, the patient’s recovery time is much faster. Patients are discharged in as little as two or three days As the heart is not fully exposed, the danger of infection is lower.
There is less bleeding and less trauma to the body and less damage to the blood cells (a possible effective of the use of a heart-lung machine). MIDCAB is available to a wider number of patients such as those who are too ill or whose hearts are too weak to undergo conventional surgery.
Valve replacement surgery is usually recommended on defects in the valve which is regurgitant (leaking). It can be repaired by reshaping the ‘leaflets’ thereby allowing the valve to open and close better. It can be performed by using a minimally invasive surgical technique. It is a particularly complex procedure which requires highly skilled and experienced surgeons.
Sometimes in the case of an enlarged aorta, it may need to be replaced. During the
aortic valve surgery, the aortic valve may be replaced. If the leaflets of the valve have tears or holes in them, they may be patched by the surgeon using tissue patches.
For patients with leaking or narrowed mitral valve, mitral valve repair is the recommended procedure. It is said to be a better option than replacement given the long-term prognosis. Cardiothoracic surgeons may perform a triangular resection in the case of a posterior leaflet prolapse. In the case of an anterior leaflet prolapse of the mitral valve, the procedure is more complex. Surgeons either use ‘goretex’ chords or do what is called a ‘chordal transfer’ (where healthy chords are transferred to the location from another part of the valve).
Here at Sri Ramakrishna Hospital, our cardiothoracic surgeons perform these procedures with great skill and dexterity. The prognosis is excellent for the patient with greater late (and early) survival, improved lifestyles, and better preservation of heart function.
The aorta is composed of the ascending aorta (the section which arises from the heart), the aortic arch (the section bending over the heart), descending thoracic aorta (the section moving down the chest region) and abdominal aorta (the part beginning at the diaphragm). Sometimes the ascending aorta has defects or is diseased and the Bentall procedure is used to correct them.
Bentall procedure in Coimbatore, is performed by cardiothoracic experts who have great skill in performing cardiothoracic procedures. In it, the patient is placed under general anesthesia and the heart is put on a heart-lung bypass machine. The section of the aorta which is diseased or defective is removed. The diseased aortic valves are also excised. The aortic root (base of the aorta) and valve are replaced. Then the coronary arteries (branching out from the ascending aorta) are re-implanted.
Conceived by Tirone David, the valve-sparing root replacement procedure allows a patient to keep the aortic valve.
A surgical treatment for aortic root aneurysms, the aneurysm is repaired while simultaneously preserving the patient’s own aortic valve. The valve itself might be repaired and re-implanted but its preservation is of great benefit to the patient in the long run by enabling the patient to avoid a lifetime of anti-coagulation therapy(among other things).
A procedure conducted on heart-lung bypass, it takes great skill and precision to carry out the valve-sparing aortic root replacement.
Closure of ASD and VSD and Intra Cardiac repair for TOF and TAPVR:
With advances in modern medicine and surgical techniques, infants born with congenital heart diseases (CHD) now have a strong chance to live long and fulfilling lives. The cardiothoracic surgeons at Sri Ramakrishna Hospital have the technology and expertise to surgically treat a number of conditions thereby ensuring that these children have the best shot at leading a normal life.
Atrial Septal Defect (ASD) repairs:
Atrial septal defect or ASD can be corrected using minimally invasive techniques or open heart surgery. In the former, a wire is inserted into a blood vessel leading to the heart. Using these two ‘clamshell’ devices are used to close the hole. In open-heart surgery the atrial septum is closed either with stitches or a patch.
Ventricular Septal Defect (VSD) repair:
Typically most small VSDs close of their own accord by the age of 1. Those which do remain need to be closed. Some which are larger or situated in more sensitive areas and require open-heart surgery. They are typically closed using a patch.
Repair of Tetralogy of Fallot (TOF):
To correct TOF open heart surgery is carried out. During the surgery, the ventricular septal defect is closed with a patch. The pulmonary valve is opened and the thickened muscle bundles are excised. A patch is placed on the right ventricle and the main pulmonary artery in order to improve the blood flow to the lungs. Sometimes a shunt procedure might be required at first. This increases blood flow to the lungs and complete correction can be done at a later stage.
Total Anomalous Pulmonary Venous Return (TAPVR) correction:
TAPVR has to be corrected within the first six months of the infant’s life. During the procedure, pulmonary veins will be routed to the left side of the heart, restoring the normal anatomy. Any abnormal connections are then closed off.
Complete A-V Canal defect correction:
In this defect there is an ASD with a VSD. There is only a single AtrioVentricular Valve. The correction of the defect involves closure of the ASD and the VSD and the division of the single AV valve into Right and Left components. Sri Ramakrishna Hospital is one of the very few Centers in the country which routinely does a single stage correction of this complex malformation.
Arterial switch operation:
This complex surgery which is done in new born babies is done for a condition called Transposition of Great Arteries. In this condition the pulmonary artery instead of arising from the right side arises from the left side of the heart and the aorta instead of arising from the left side originates from the right side. By this complex procedure namely Arterial Switch Operation the position of these both blood vessels are interchanged thereby restoring the normal anatomy.
Fontan procedure
This fontan procedure is performed when there is a complex deformity of the heart and requires a single chamber palliation. At Sri Ramakrishna Hospital cardiothoracic surgeons perform these complex surgeries in children who have complex anatomical malformations which are not totally correctable.