- Home
- About Us
- Doctors
- Centre Of Excellence
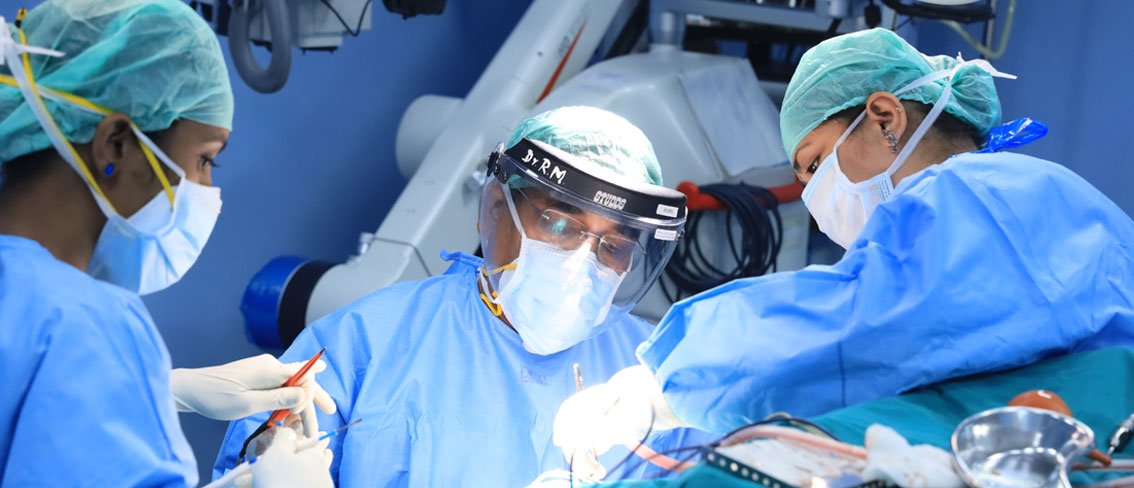
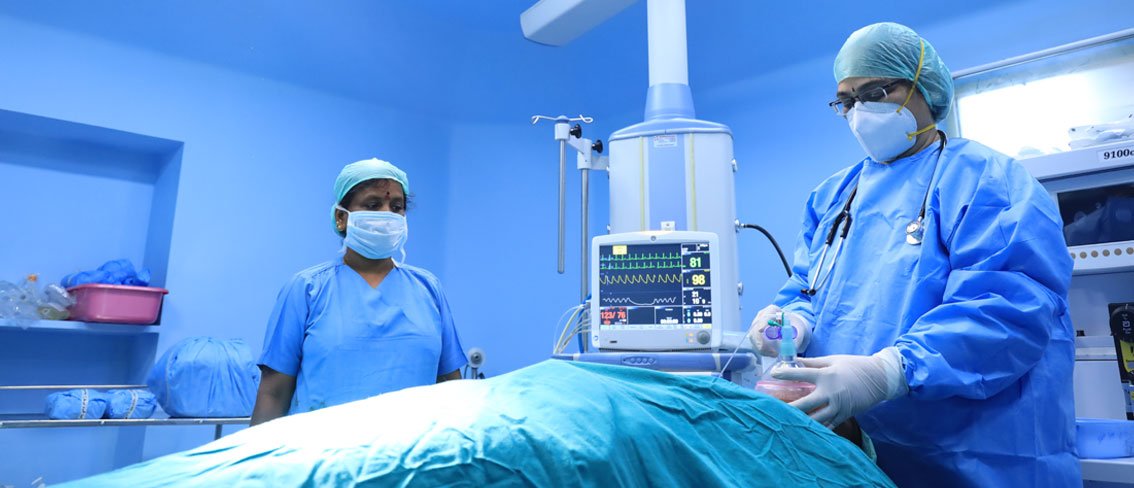
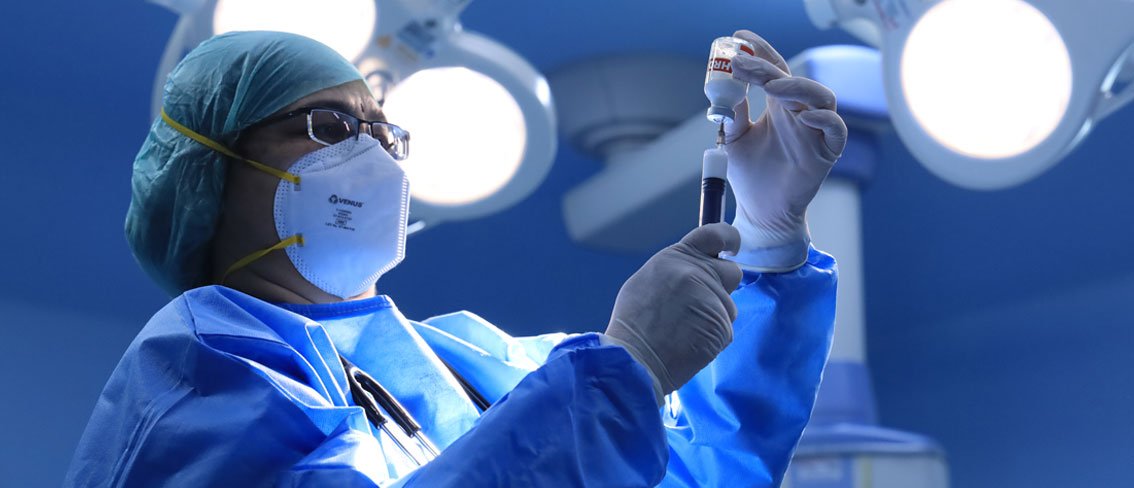
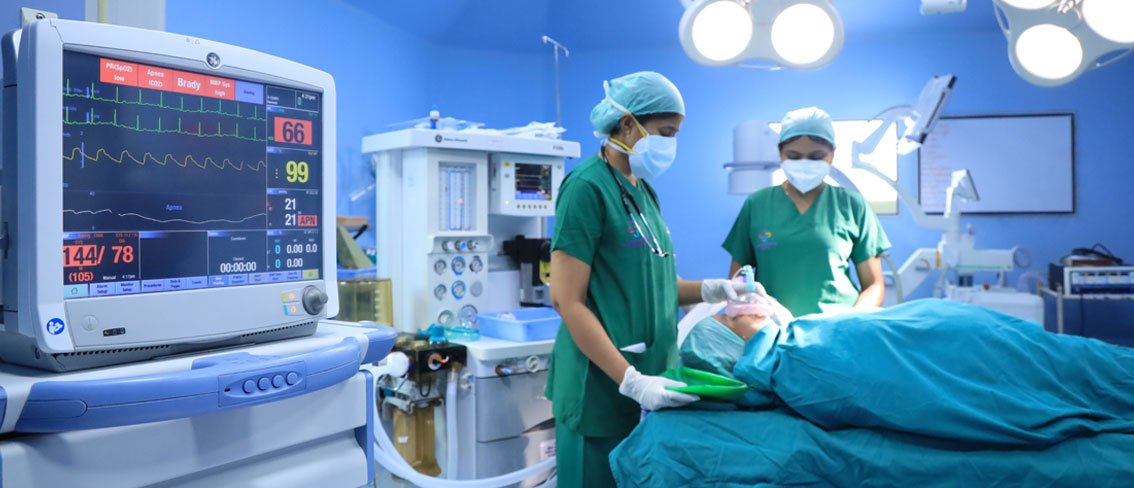
- Anesthesiology
- General Medicine
- Neurology
- Pediatrics
- Breast and Endocrine Surgery
- General Surgery
- Neurosurgery
- Physiotherapy
- Cardiology
- HPB, GI Surgery & Liver Transplant Unit
- Obstetrics & Gynaecology
- Plastic & Hand Surgery
- Cardiovascular and Thoracic Surgery
- In Vitro Fertilisation (IVF)
- Oncology
- Psychiatry
- Clinical Haematology
- Intensive Care Unit (ICU)
- Ophthalmology
- Pulmonology
- Clinical Laboratory
- Interventional Radiology
- Orthopaedics
- Radiology And Imaging
- Dentistry
- Maxillofacial Surgery
- Pain Management
- Rheumatology And Clinical Immunology
- Dermatology
- Medical Gastroenterology & Hepatology
- Pediatric Cardiac Surgery
- Transfusion Medicine
- Diabetology and Endocrinology
- Medical Genetics
- Pediatric Cardiology
- Uro & Cosmetic Gynaecology
- Emergency Care
- Neonatology
- Pediatric Endocrinology
- Urology
- ENT
- Nephrology
- Pediatric Intensive Care Unit
- Vascular Surgery
- Facilities
- International Patients
- Health Packages
- Academics
- Contact Us